Hepatitis C: Indigenous
Related Resources
Booklet: Frequently asked questions about hepatitis C
 Simple answers to questions most often asked by people with hepatitis C (14 pages).
Simple answers to questions most often asked by people with hepatitis C (14 pages).
May is Aboriginal hepatitis C awareness month!
Basic facts about hepatitis C
(video transcript)
What is hepatitis C?
It’s a virus that can cause damage to the liver, an organ that has many different functions essential to your life.
How many people in Canada have it?
About 300,000 people in Canada have hepatitis C. That is about 1 in every 100 people.
Many people don’t know they have it.
Of the estimated 300,000 people living with hepatitis C in Canada, almost half do not know they have it!
Can the body get rid of the infection?
Sometimes, yes. For every 10 people that get hepatitis C, about three will be able to get rid of the infection in the first six months. Their body attacks the virus and gets rid of it naturally.
About 7 will have chronic hepatitis C. That is, they will likely have it for life, unless they get treatment.
Can hepatitis C be cured?
Yes! With new medications about 9 people out of every 10 who complete treatment may be cured.
Rates may differ for those who are also living with HIV.
Is there a vaccine for hepatitis C?
No, there is no vaccine to protect you from getting hepatitis C. You can protect yourself by knowing how it is passed and taking actions to reduce the chance of getting hepatitis C.
If I get hepatitis C, will I know I have it?
Unless you know what activities can put you at risk of getting hepatitis C, you will probably not know you have it. This is because most people do not have symptoms right away.
Only about 1 in 4 people have symptoms when they first get the virus. Many people do not have symptoms for 10 to 30 years after getting hepatitis C.
This is because the liver can keep doing its job for a long time, even when it is damaged.
Sorting out the symptoms
Many people with hepatitis C are living with more than one condition. This can make it difficult to sort out which symptoms are related to hepatitis C.
See your health care provider if you are having symptoms that you are concerned about.
What are the symptoms of hepatitis C?
Early on, most people will have no or few symptoms, but over time, some may experience:
- feeling tired
- muscle or joint pain
- headaches
- itchy skin
- depression
- anxiety
- abdominal pain in and around the liver
- brain fog (in other words, having a hard time concentrating and suffering from memory lapses)
Related Resources
Booklet: Frequently asked questions about hepatitis C
 Simple answers to questions most often asked by people with hepatitis C (14 pages).
Simple answers to questions most often asked by people with hepatitis C (14 pages).
Page: HIV, HBV, and HCV can be passed through…[COMING SOON]
Compare through which body fluids HIV, HBV and HCV can be passed.
How hepatitis C is passed?
(video transcript)
Importance of understanding how hepatitis C is passed
After learning about hepatitis C, some wonder if people they know have it. But, you cannot tell from looking at a person if they have hepatitis C.
This is why it is important to know how hepatitis C is passed and how it is not passed. Then you can take actions to try to protect yourself or others from getting hepatitis C.
Hepatitis C is not passed through…
…regular day-to-day activities like: coughing, hugging, kissing, or sharing dishes. These day-to-day activities, and others like them are safe.
How to prevent passing hepatitis C
You can get hepatitis C if the blood of a person who has the virus gets into your blood. Some activities are more likely to lead to blood-to-blood contact than others.
The greater the chance of blood-to-blood contact, the greater the chance that hepatitis C will be spread.
Today, hepatitis C is most often passed…
…when people share or re-use drugs or injection drug equipment. If the drugs or injection equipment are used for more than one person, there is a high chance for hepatitis C to pass from someone who has the virus to another person.
This is why injecting supplies (like syringes, water, spoons/cookers and cotton) are sometimes supplied free of charge to people who inject drugs. Otherwise, if people share injection equipment they have a high chance of getting hepatitis C.
Because it is so easy for hepatitis C to get into the bloodstream through any kind of injection, all medical procedures must be done using new disposable syringes and sterilized equipment.
Hepatitis C can sometimes be passed…
…when the blood of an infected person comes into contact with another person’s body through an opening in the skin.
For example, hepatitis C can get into the body through:
- using unsterile, re-used or shared equipment during tattooing, body piercing or ceremonial activities, for example, Sun Dance ceremonial piercings
- by re-using or sharing non-injection drug equipment, like straws or crack pipes
It is also possible for hepatitis C to be passed…
- from sharing personal tools that could have blood on them like razors, toothbrushes or nail clippers
- from medical or dental procedures if the equipment is reused and has not been properly sterilized
- by accidentally being poked with a used needle, or
Although it doesn’t happen very often, it is possible for hepatitis C to spread from a mother to her baby at birth.
Can hepatitis C be passed through sexual contact?
The risk of hepatitis C being passed through sexual contact is zero to low, but …the risk goes up if blood is present, even if you can’t see the blood.
Examples of situations when blood is more likely to present include:
- the presence of infections like HIV, hepatitis B
- the presence of other infections or conditions, like herpes, that cause sores or cuts
- unprotected sex where there may be tearing, such with anal sex, “dry” sex, or sexual assault. (In the case of sexual assault, the victim and the perpetrator are at risk), and
- unprotected sex during menstruation
Related Resources
Patient Page: Tests used for diagnosing hepatitis C
This patient page explains the hepatitis C testing process (with diagram).
Provider Page: Hepatitis C Virus Pre- and Post-test checklists
 Discussion checklists for providers to use with patients before/after the antibody and RNA tests.
Discussion checklists for providers to use with patients before/after the antibody and RNA tests.
Getting tested for hepatitis C
(video transcript)
Should I get tested to see if I have it?
You should get tested if you have had even one event where hepatitis C could have been passed, whether the event was long time ago or recently.
For example, you should get tested if:
- you have ever re-used or shared any type of drug equipment, or
- if you have ever had a medical procedure in a country that does not properly sterilize medical equipment, or
- if you had a blood transfusion in Canada before 1992, before blood was screened for hepatitis C.
These are just some examples of risk events. If you are not sure if you should get tested for hepatitis C, talk to a health care provider.
Getting your blood tested is the only way to know for sure if you have or do not have hepatitis C.
How do I get tested?
You can go to any health care provider, like a nurse or doctor, to ask about how and where to get tested for hepatitis C.
How many types of blood tests are often done to find out if a person has hepatitis C?
Two types of blood tests are often done to find out if a person has hepatitis C. These tests are usually taken at different times, but this depends on where you live. So it is important to know what these tests mean.
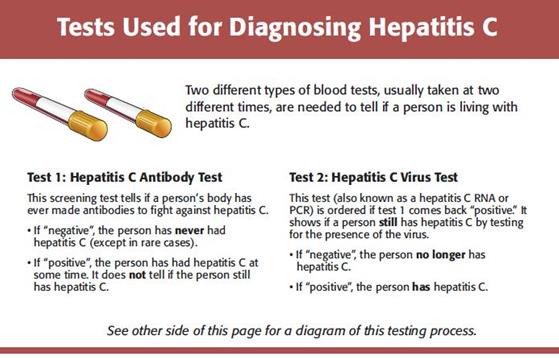
What is the first test?
If you are getting tested to see if you have hepatitis C, the first test you will get is the hepatitis C antibody test. This test shows if you have ever had hepatitis C. It does not tell if you still have it.
What if the first test is “negative”?
If the first test, the antibody test, is negative, it means that hepatitis C antibodies were not found and you have never had hepatitis C. You do not need to get the second blood test.
What if the first test is positive?
If the antibody test is positive, hepatitis C antibodies were found and you have had hepatitis C at some time. This test does not tell if you still have it so you will need the second test.
What is the second test?
The next test is the hepatitis C virus test (also known as hepatitis C RNA or PCR). This second test checks to see if you are still have hepatitis C.
What if the second test is negative?
If the hepatitis C virus test is negative, the hepatitis C virus was not found so you no longer have hepatitis C.
It is possible to get hepatitis C more than once. So you may want to talk to a health care provider about how to prevent getting hepatitis C again.
What if the second test is positive?
If the hepatitis C virus test is positive, the hepatitis C virus was found. This means you have hepatitis C.
Your test result must be sent to your local public health department so they can count how many people have hepatitis C.
However, your hepatitis C diagnosis is kept confidential. You are not required to tell anyone that you have hepatitis C. You can choose who to tell.
Related resources
Patient Page: Questions people frequently ask their providers about hepatitis C
 A checklist of questions people frequently ask their health care providers about hepatitis C.
A checklist of questions people frequently ask their health care providers about hepatitis C.
Patient Page: “Personal bill of rights”
 This “personal bill of rights” may help you to speak up for yourself.
This “personal bill of rights” may help you to speak up for yourself.
If I have hepatitis C, what should I know and what’s next?
(video transcript)
What does hepatitis C do to the body?
Hepatitis C can cause swelling and scarring in the liver. After 20 to 30 years, the liver can become quite damaged and unable to work properly. This can cause many different health problems because the liver does so many important jobs for the body.
Anyone with signs of liver damage should be checked to see if they can get hepatitis C treatment as it could stop further liver damage.
How can I know if my liver is damaged?
Health care providers cannot predict who will have liver damage, so it is important to regularly see a provider who can monitor your health.
Your health care provider can complete a detailed health assessment. This assessment will help to find out if the hepatitis C infection has caused any problems in how well your liver works. It may include:
- a physical examination
- blood tests, and
- other tests, like a Fibroscan
Questions to ask your health care provider
It is important to ask your provider for more information about:
- hepatitis C
- treatment for hepatitis C
- deciding who to tell that you have hepatitis C
- how you can stay healthy, and about
- vaccinations such as hepatitis A, B, pneumonia, and influenza
These vaccinations are free for people living with hepatitis C. You can get these vaccinations from your health care provider or public health unit.
Getting information about hepatitis C
There are many sources of hepatitis C information such as the internet, friends & family, and health care providers. Information can sometimes be out of date or incorrect.
It is important to check out the information and decide if the information is helpful in your situation.
When should I see a specialist/or go to a liver clinic?
People often see a specialist or go to a liver clinic when thinking about going for hepatitis C treatment. You may need a referral from your health care provider to see a hepatitis C specialist or to go to a liver clinic. With newer drugs that have fewer side effects, treatment may be available from other providers.
Also, you may want to speak with a specialist or a pharmacist if you are considering alternative therapies, herbal remedies or traditional medicines. These specialists may be able to determine what ingredients would be safe for you.
Do people living with hepatitis C need to see a health care provider even if they feel fine?
Yes. They should see their provider every 6 to 12 months. Even if a person feels well and has no symptoms, hepatitis C can still be damaging their liver.
Deciding who to tell
Sometimes people newly diagnosed with a disease that can be passed to others do not want to talk about it. They are not sure how others will react.
For example, many people don’t know much about hepatitis C, so those living with it worry that friends or family will become overly cautious or afraid of catching it.
Before telling others that you have hepatitis C, take your time to think about it. There is no rush, but it is important to have some friends or family know so that you can have their support. When deciding who to tell, ask yourself:
- who will understand
- who can I trust to respect my privacy and feelings
Understanding stigma
Stigma happens when somebody is judged or not valued as a person. People with hepatitis C sometimes feel judged or not valued because they have hepatitis C.
Stigma can happen for many reasons; one reason can be fear that comes from a lack of knowledge. People may be afraid because they don’t know about how hepatitis C is spread from person to person, how it affects health or how it is treated.
Getting the healthcare you need
It’s important to get the health care you need but it can be hard to ask for it.
This “Personal Bill of Rights” is one support that might help you to speak up for yourself.
Related Resources
Patient Book: Using your voice
 A skills building workbook to help people get the care and support they need (25 pages).
A skills building workbook to help people get the care and support they need (25 pages).
Patient Card: Tips to getting your message heard
 6 tips on how to get people to hear you and what to do when people say “no.”
6 tips on how to get people to hear you and what to do when people say “no.”
Healthy balance
(video transcript)
Finding a healthy balance
Learning to balance a chronic disease like hepatitis C with other things going on in your life can take time. You may have to juggle several different priorities all at once.
Deciding what to do first and how much time to spend on each thing will depend on your situation.
Staying healthy
To help keep your physical and emotional life balanced, try to:
- Stay connected. Having a chronic infectious disease can affect your social life and leave you feeling isolated.
- Figure out who you feel comfortable talking with. It is helpful to have someone who you can talk to about what you are going through and the decisions you need to make.
- Reduce physical and emotional stress with exercise and eating a balanced diet.
Alcohol
Alcohol can speed up liver damage. Talk to your provider about alcohol use, how it can affect the liver and the treatment of hepatitis C, and if you need to cut down on alcohol use.
Supplements
Tell your health care provider everything you are taking. Some people use herbal remedies, other supplements, over-the-counter drugs, or traditional medicines.
Some supplements or other medicines can be harmful for your liver when taken alone or with medicine prescribed by your provider.
Food
Most people with hepatitis C do not need a special diet. A balanced diet as outlined in Canada’s Food Guide can help maintain health.
This includes eating a variety of nutritious food – things like vegetables and fruits, whole grains, meat and alternatives, and milk products.
You may need a special diet if you have liver damage. In these cases, speak to your health care provider or nutritionist to learn about what you need to eat and what to avoid.
Related Resources
Video:Getting ready for hepatitis C treatment
 This video outlines what often needs to be done to get ready for hepatitis C treatment (5 min.)
This video outlines what often needs to be done to get ready for hepatitis C treatment (5 min.)
Treatment
(video transcript)
What are the current treatments?
Current treatments are very different from old therapies that included interferon. They:
- usually take 8 to 12 weeks
- involve only oral treatments, such as pills or tablets instead of injections,
- have much fewer and less severe side effects
- and have cure rates higher than 95%
Hepatitis C treatment is available across Canada, but speak to a health care provider to find out details for your province/territory.
It is important to remember that being cured does not protect you…
from getting hepatitis C again.
Only protecting yourself from contact with blood will protect you from getting a new hepatitis C infection.
Protecting yourself from contact with blood will also decrease the chance of getting other blood-borne infections.
But, keep in mind that some infections, like HIV and hepatitis B, are passed through blood AND other body fluids.
Will I get treatment?
Check with a health care provider to discuss if you need treatment, when is the best time to get treatment, as well as other treatment options.
The type of treatment you get can depend on many things. For example, treatment options may depend on:
- the type or strain of hepatitis C you have; also known as a genotype
- your health as well as the health of your liver, such as how much swelling and scarring there is
How do I get treatment?
Different providers can give hepatitis C treatment. Often it is given through a specialist or at a liver clinic, but this can take time as there are sometimes several steps involved:
- first you need to see a regular health care provider, like a nurse or a doctor
- this provider may refer you to a specialist or a liver clinic
- you will see a specialist or go to a liver clinic to discuss treatment and then
- get ready for treatment; this can mean seeing other providers to help get your mind, body, spirit and life ready
- once your mind, body, spirit and life are ready, then treatment may begin
Drug-to-drug interactions
It is very important to talk with your provider about drugs or supplements that might interact with hepatitis C treatment drugs.
Some drugs, herbal or traditional medicines, when taken with hepatitis C treatment drugs, can cause serious reactions or lower the chance that the hepatitis C treatment will work.
What to avoid depends on what type of hepatitis C treatment you are taking, but examples include:
- Some heart medications
- Birth control containing estrogen
- Sleep medication with Benzodiazepines
- Herbal or traditional medicines (for example, St. John’s wort)
- Allergy and cold medications that contain antihistamines
It is important to speak with your health care provider to find out what drugs need to be avoided because this will depend on the type of hepatitis C treatment you get.
Getting ready for life after treatment
People often make many changes before and during treatment. For example, they might gain support networks of friends and health care providers, or make changes to diet and physical activity. But what will happen after treatment ends?
Talk with your team about life after treatment
Here are some things for you and your care team to talk about:
- Will my care team change?
- Will I need to change my supports?
- Am I emotionally ready if treatment doesn’t work?
- If treatment does work, will I feel better right away?